Prolapsed Lumbar Intervertebral Disc- medical management
The prolapsed lumbar intervertebral disc also referred to as slipped disc, sciatica, or just disc prolapse is a painful condition where pain starts in the lower back or buttocks and travels like a wave towards the affected lower leg up to the heel a condition often referred as sciatica.
A disc is an oval structure located between the two vertebral segments of the vertebral column. Thus there are 23 functional intervertebral discs, each disc connecting the inferior surface of the upper vertebra to the superior surface of the vertebra below. A healthy disc has an outer tough ring made of a fibrous structure arranged tightly in a circular fashion and attached strongly to the outer part of the adjacent vertebral surfaces is called the annulus. It has a central soft and gelatinous but tough tissue called the nucleus pulposus. The nucleus pulposus remains confined within the boundaries of the annulus and does not allow the nucleus to come out and works as a shock absorber.
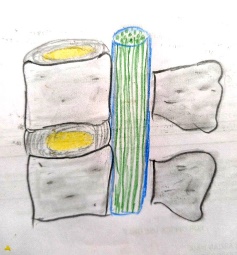
Annulus (blue arrow), nucleus pulposus(yellow), nerves of spinal cord (red arrow),
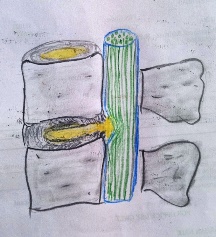
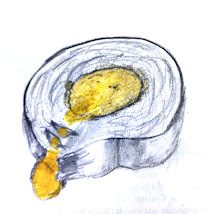
Rupture of nucleus pulposus(yellow) through the cracks in the annulus causing nerve compression

An intervertebral disc works like a shock-absorbing spring
Causes of disc prolapse or slipped disc- Due to constant wear and tear and minor trauma stresses buildup in the annulus which together with dehydration caused by aging-related degeneration leads to cracks in the layers of the annulus. Over the years and /or acute trauma such as lifting weight or sudden jerk causes nucleus prolapses to herniate out of the boundaries of the annulus through the cracks and enter into the spinal canal causing pressure on the spinal cord or spinal nerves. This causes pinching of spinal nerves and symptoms. Other causes of slipped discs include sudden lifting of weight, jumping, falling, accidents, and getting jerks while playing ball games. Bending forward causes maximum stress on the discs and if the person attempts to lift a heavy object from the bent position the force may lead to the rupture of the intervertebral disc.
Symptoms-
The commonest presenting complaint is low backache ranging from mild to moderate severity starts gradually and progresses to severe pain over the weeks or months. A classic case of disc prolapse presents with pain and /or tingling in the low back, and buttocks radiating to the back of legs, heels, or toes. If the nerve is pinched severely the patient may get weakness in the foot on the affected side. This may force the patient to limp or stoop forward while walking.
Some patients notice the appearance of heaviness, tingling, and pain in legs associated with imbalance after walking a certain distance. Sitting down for rest gives them immediate relief and the patient can walk once again till he gets similar symptoms after walking the same distance. This condition is called Neurogenic claudication.
Examination finding - Such patients show positive straight leg raising test (patient perceives pain along the back of lower limb while the leg is raised passively in a straight position), muscle spasms in the paraspinal area, tenderness in the lumbar spine, weakness of the foot or toes on the affected side, and reduced sensation in the area of the affected nerve. In severe and long-standing cases there may be wasting of the leg’s muscles.
Treatment of slipped disc: Once the disc is prolapsed (herniation–as it is called) it does not go back to its original position. Follow-up MRIs of some patients showing the resolution of the disc is due to its shrinkage or adsorption.
Important steps in the first line of management of acute slip disc--
- Patient should be put on total bed rest for 3-5 days
- Cold fomentation with ice should be applied on the back
- Non-steroidal anti-inflammatory medicines are the drug of choice such as Paracetamol, Ibuprofen, Diclofenac sodium, Naproxen, and Aceclofenac.
- Some patients are benefited from small doses of steroids.
- Application of local liniments at the painful site works as a counterirritant and often gives good relief.
- A small dose of night sedation with Alprazolam or Clonazepam is helpful.
However severe or acute the symptoms are on the first day more than 90% of patients get good relief with the first line of treatment. Once the acute symptoms are relieved the patient is gradually mobilized with the help of a trained physiotherapist. They are encouraged to do moderate stretching exercises of spinal and leg muscles and go to work in 8-10 days.
During further follow-up, the physiotherapists encourage patients to strengthen the core muscles of the abdomen and lumbar spine.
Some patients come back with recurrence of symptoms usually due to some exertion or minor trauma and are benefited by repeating the first line of treatment.
Recurrent chronic backache and sciatica- the commonest cause of absenteeism from work belong to this group. Such patients are best treated by physiotherapists. It involves
- Traction of the lumbar spine- The weight of traction should be up to one-third of the body weight or less as tolerated to be given for a week. I prefer static traction to dynamic traction to achieve an effective traction effect. Turning the body posture to right, left, and prone during traction may give more benefits.
- IFT- Interferential Therapy sends low-frequency electrical stimulation to the affected muscles and nerves in the body. It helps improve blood circulation to the affected area and gives good relief to many patients.
- Manipulation- This is apparently done to “realign” the joints of vertebrae. During manipulation, the patient’s head, neck, and spine are twisted, pulled, and jerked to achieve alignment. Often this produces cracks and pops sounds from the joint. Most commonly this is done by chiropractors who are not medical practitioners but are very popular in society.
Although this method has not been approved by the medical world, many patients swear by it and claim good relief. Critics argue that such vigorous manipulations without knowing the anatomy or disease in the spine could be dangerous and may cause more harm.
- Hot / Cold Therapy- In acute back pain ice packs help relieve pain. Initially uncomfortable for a short time till the area becomes numb and pain is relieved. It can be applied many times in a day. Hot fomentations are good for chronic backache it is effective in relieving muscle spasm.
- Braces or lumbosacral belt helps to support the spine and gives pain relief by stabilizing and compressing the painful muscles. It is advisable not to use these external braces for more than a few weeks.
Investigations
Patients who continue to suffer disabling pain despite all the physiotherapy measures need to be investigated for the cause of pain. Investigations-
X-ray of lumbosacral spine- radiograph of the spine does not show evidence of intervertebral disc prolapse, however, it may suggest such a possibility by reduction in the height of the intervertebral disc space and formation of bony outgrowth along the vertebrae called osteophytes.
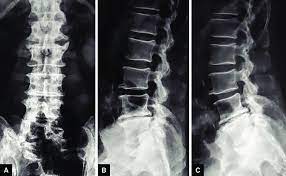
Reduction in disc height suggests disc pathology (thin arrow), formation of bony outgrowth osteophytes (short arrow)
MRI of the spine- This is the gold standard modality that shows the health of discs, their rupture,
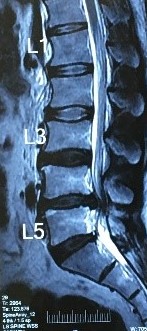
A healthy disc looks grey-white (thin red arrow), degenerated disc looks dark black (yellow arrow), and Prolapsed disc compresses the nerve (thick red arrow)
and prolapse along with the state of the pinched nerve. In addition, it also reveals the presence of other pathological processes in and around the vertebrae which could contribute to the symptoms.
In advanced situations, patients develop numbness, weakness, and disturbing tingling in the legs. Such patients can’t walk or stand for more than a few minutes. Findings of the X-rays and MRI are interpreted in light of the patient’s condition. If the disc pathology is considered to be the cause of suffering the patient is encouraged to undergo surgical treatment.
Dr. Dilip Kiyawat
Consultant Neuro and Spine Surgeon
Jehangir Hospital, Pune
9822046043